Yesterday I was interpreting for our hand therapist. She was putting bilateral (this and other obscure English words discussed below) splints on a young man. (Some patient details changed to protect privacy.) “The next splint is here,” she said. Great, I thought, looking around—where? I’ll grab it for her. I didn’t see a splint, though. “Where is it?”, I asked her, somewhat puzzled. She watched me look around. “No—there’s someone else coming in to get a splint, and he’s here.” Ahah—metonymy. More on this later, but first, let’s talk about those splints—and that hand therapist.
I’m in Guatemala at the moment, with a group called Surgicorps. We’re a team of all-volunteer surgeons, anesthesiologists, nurses, technicians, therapists, and assorted non-medical personnel, such as myself—I’m an interpreter. There are lots of groups like ours that come here to Guatemala—there’s an enormous need for surgical care, and not a lot of options for getting it for the very poor population that we serve.
What makes us special: among other things, it’s the fact that we have a hand surgeon. Hand surgery is a very specialized occupation—in the course of learning his trade, our hand surgeon did fellowships in both plastic surgery and orthopedics. A fellowship is about five years, and that’s on top of four years of college, four years of medical school, and a three-year residency—so, these guys are hard to come by.
As specialized and as in short supply as the hand surgeons of the world are, there’s another profession that’s even harder to find an expert in: hand therapists. Hand therapy is a subfield of occupational therapy, which is the art and science of teaching people how to function normally after things like strokes, heart attacks, and amputations. The other day, one of the physicians said to me: The first time I went on one of these missions, I heard that we had a hand therapist with us, and I thought: why the hell do we need one of those? What could she possibly do on a surgical trip? Then I saw her working, and I realized: she’s more important than the physicians.
Almost every kind of hand surgery requires some kind of splinting afterwards, and it’s to the extent that the splinting is or isn’t successful that the surgery is or isn’t successful. For example: an operation that our hand surgeon does here quite frequently is repairing something called syndactyly. Syndactyly is a condition in which fingers don’t separate from each other during development in the womb. It’s ruinous here in Guatemala, where most people’s educational opportunities are nil, and the only option for earning a living for most people is manual labor.

Our hand surgeon can undo the syndactyly. Typically what happens in syndactyly is that the genes that should cause the tissue between the fingers in the fetal hand to reabsorb don’t work right, and what the surgeon does is to cut that tissue away, and then graft some skin between the fingers. (I’m simplifying the description of the surgery!) Once that surgery is done, though, those fingers have to be kept apart for several months. Otherwise, the fingers will re-fuse. How you keep that from happening: a hand therapist builds you a special kind of splint. These have to be made to order after the surgery, as they have to fit the individual child very well, and they have to fit that child when he has bandages on his fingers after the surgery. (That’s why you can’t do it before the surgery.)
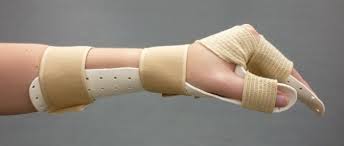
The surgery to repair syndactyly is usually done when a child is small. So, here’s what it’s like to fit one of those custom-made splints after surgery: you’ve got a little kid. The kid is coming out from under anesthesia and is disoriented, nauseous, surrounded by funny-looking people speaking a language that he can’t understand—and he’s scared shitless. So, you’re trying to build a very precisely-sized splint for a kid whose hand you need to fit it to—while he cries, and screams, and tries to pull his arm away from you, and tries to make a little fist while you’re trying to get things between his fingers. Add to the mix the fact that the splint is made from a kind of epoxy that is rigid when cool, and flexible when heated. You heat it up, then take it over to the kid and try to mold it to the right size while he cries, and screams, and tries to pull his arm away from you, and tries to make a little fist while you’re trying to fit it between his fingers. The resin cools down while you’re trying to do your thing, and then it won’t bend any more? Tough shit—go back to your heat source, heat it up again, and then try again.
So: the surgery doesn’t work without a good hand therapist. Being a hand therapist is a difficult job to do, and it’s hard to find places to learn to do it, and in addition to having considerable technical skills in order to make the splints correctly, you need to be able to do it under very adverse conditions, and to keep your cool while you’re doing it. Indeed, it’s the hand therapist that is the key to our mission. We can replace a surgeon, or an anesthesiologist, or a nurse—or an interpreter—but a good hand therapist is hard to come by.
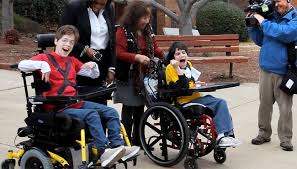
So, back to the young man and “the next splint:” he has cerebral palsy. This means that he has essentially no control over his muscles whatsoever. They twitch, and cramp, and they make his hands clench into useless fists that can’t be opened. He can’t speak. He can’t nod his head “yes,” or shake it “no.” Our hand therapist was making splints for the young man that would keep his hands open for half of the day. If they can stay open, he will be able to grasp things. This is a smart teenager who can’t hold so much as a pencil—having hands that function even a little bit would be life-changing for him. Can the hand surgeon make this happen? No—it’s only the hand therapist who can give him that new capacity, one that you and I probably never even think about.
So, “the next splint is here:” this is an example of a phenomenon called metonymy. Metonymy is the process of referring to something by one of its attributes. For example:
- The hamburger in the corner is a slob and needs more napkins. Meaning: the person who is eating a hamburger and is in the corner is a slob, etc.
- Would you ask if the right front flat in bay two is also supposed to get an oil change? Meaning: there’s a car that has a right front flat in bay two, and I need to know if it’s also supposed to get an oil change.
This is a different phenomenon from metaphor, in which we refer to something as something else entirely—love is a river, life is a journey, for example—as opposed to referring to it by some attribute that it has—the hamburger that the sloppy customer has, or the flat tire that the car has, or whatever. Metonymy is a super-common phenomenon in language that lets us take advantage of context in the course of communication—and not just linguistic context, but what you could think of as “world” context, and from a theoretical point of view, that’s pretty interesting, for the following reason. Most linguistic theories are entirely about language and its structure (I’m simplifying here—if you’re a sociolinguist, please don’t send me hate mail), and if you need to incorporate the world into your theory about how language works, that’s quite a challenge. Being context-dependent, it also requires that both the speaker and the hearer know what that context is—I didn’t know that the therapist had another patient scheduled, so I totally misunderstood her statement, thinking that she was referring to an actual splint, not to a person who was going to receive a splint.

Back to the kid again: he went home happy, him and his mother hopeful that next year his hands will be more functional. We’re talking about a kid who is super-happy to be spending his days in a wheelchair, because it means that he’s not spending his days in bed. (How’s your day going, dear reader?) If he gets some improvement over the course of this year, then when we come back with a hand therapist again next year, he can improve even more with another splint. Someday he might be able to hold a pencil and use writing to get all of the stuff that’s in his head out of it, like I do—he sure as hell isn’t ever going to be able to speak.

Here’s the thing: if there’s no Surgicorps, then there’s no hand therapist, and there’s no hope for functional hands for that kid—a teenager with a fully functional mind and not a lot of physical abilities. (OK: no physical abilities.) One of our hand therapists is Courtney Retzer Vargo. Courtney has a PhD in occupational therapy, two kids, a hot husband, and a busy job in the United States. But, every so often she burns up a week of her hard-earned vacation time and flies to Guatemala or Zambia to volunteer a week of her time doing exactly this. Like all of us in Surgicorps, she buys her own plane ticket, pays for her own food and lodging–contributes a week of hard-earned vacation time. Surgicorps pays for all of the costs of the patients’ treatments, and Surgicorps lives or dies on the basis of donations from nice people like you. Click on this link, and making a donation will take you less than 5 minutes. $250 will pay all surgical costs for one patient, or the expenses for transportation and lodging for a patient and their parent during the period of the surgery. (See this post for what that trip is like, and why they need us to put them up.) $100 will pay for four surgical packs. $10 will pay for all of the Tylenol that we’ll send our patients home with this week—and, yes, our patients go home with nothing stronger than that. Do it—if you don’t feel better about life immediately, I’ll give you your money back—and you know where I live!
English notes:
- Bilateral: on both sides. Bilateral symmetry is one of the most common features of multi-celled animals. How it was used in the post: She was putting bilateral splints on a young man.
- To be hard to come by: to be difficult to obtain. During a famine, there actually is usually food, but it’s very expensive and hard to come by. How it was used in the post: Indeed, it’s the hand therapist that is the key to our mission—we can replace a surgeon, or an anesthesiologist, or a nurse—or an interpreter—but a good hand therapist is hard to come by.
- Physician: a somewhat technical or formal term for doctor, and specifically, a medical doctor. Non-health-care people don’t use it very often, but health care professionals use it frequently—especially doctors. 🙂 How it was used in the post: The other day, one of the physicians said to me: The first time I went on one of these missions, I heard that we had a hand therapist with us, and I thought: why the hell do we need one of those? What could she possibly do on a surgical trip? Then I saw her working, and I realized: she’s more important than the doctors.
Spanish notes:
- Férula or tablilla: a splint. I’ve noticed over the course of the past four years that some people know one word, some people know the other, and many, many of them don’t know either. In that case, I ask the therapist if I can tell the patient that a férula is a piece of hard plastic that will keep their fingers apart/fist from closing/wrist from moving/whatever.
French notes:
- une attelle: a splint. I think there’s also a word une éclisse, but I haven’t been able to verify that one.
“Une attelle” is a “une éclisse” when it is a medical “éclisse” . Une attelle has a wider field of applications .
LikeLike